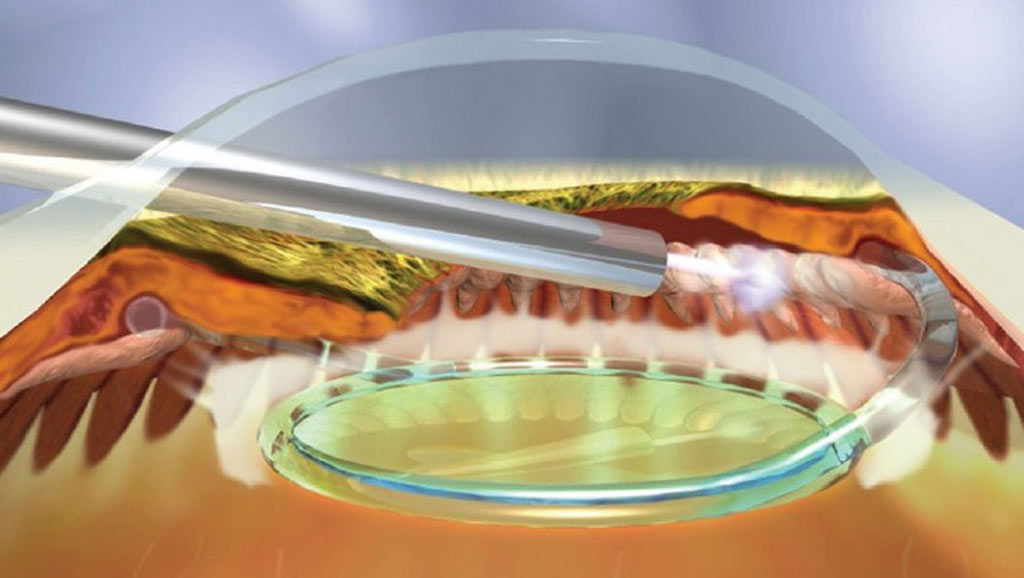
Endoscopic Cyclophotocoagulation
FAQ
Frequently Asked Questions
Endocyclophotocoagulation (ECP) is a laser treatment to lower intraocular pressure (IOP) and reduce the need for eye drop medications.
ECP is a laser probe that targets the ciliary body which is the part of the eye that produces fluid that is partially responsible for your IOP. The ciliary body is located behind the colour of the eye (Iris). You cannot see it directly.
There are other forms of treatment targeting the ciliary body to reduce IOP (fluid production). However, the ECP treatment is unique as the laser probe is inserted inside the eye via a tiny incision; usually at the same time as cataract surgery. The advantage of ECP over other cycloablation procedures, such as cyclodiode, is that your doctor can visualise the ciliary body directly during the treatment, theoretically improving accuracy. ECP treatment has to be performed in the operation room under sterile conditions.
Inside the eye, a clear watery fluid called aqueous is produced by a part of the eye called the ciliary body which is located just behind the coloured part of the eye (iris). The clear fluid circulates inside the eye before draining away through drainage channels. In glaucoma, these drainage channels do not work properly and this can cause a build-up of pressure inside the eye. This pressure can damage the optic nerve which carries images from the eye to the brain affecting your vision.
High eye pressure occurs when more fluid is produced than can drain away. This procedure delivers laser energy to the ciliary body, causing a reduction in fluid production, thereby lowering eye pressure. The procedure reduces fluid inside the eye, which is separate from tears.
The ECP treatment will not permanently reduce the fluid production as the ciliary body can grow back after ECP or any external laser (micropulse or traditional diode laser) or ultrasound (HIFU) treatment. The ECP treatment can be repeated, if necessary.
ECP is suitable for patients with moderate glaucoma who either have had cataract surgery or will be undergoing cataract surgery.
ECP alone is not suitable for advanced glaucoma or normal tension glaucoma. However, it can be performed as an adjunct to other glaucoma surgery such as aqueous shunt insertion, if the latter is not enough to reduce eye pressure.[1] It is not recommended to perform ECP at the same time as other glaucoma surgery, as the risk of extremely low pressure (hypotony) is high.
ECP should not be performed if you have never had cataract surgery and have excellent vision, as ECP will inevitably lead to cataract development.
ECP helps reduce eye pressure and the need for glaucoma eye drops. However, the eye pressure lowering effect of ECP may reduce over time and you may need to resume using glaucoma medications or to repeat the treatment. A US study has shown that combined ECP and cataract surgery lowers eye pressure about 3 mmHg more than cataract surgery alone.[2]
In a particular type of glaucoma called angle closure glaucoma, where the natural drainage angle of the eye is closed, ECP combined with cataract surgery can help further open up the drainage angle in addition to lower eye pressure.[3]
ECP will not cure your glaucoma, reverse any damage already caused by glaucoma, or bring back any lost vision.
ECP treatment takes about five minutes and is performed at the end of cataract surgery. The ECP laser probe is equipped with a camera allowing your doctor to visualise the area of treatment. The operation is usually performed under a local anaesthetic, meaning that you are awake but your eye is numb so you will not feel anything.
The ECP should work straight away to lower your eye pressure, however you may still need to continue some glaucoma medication in the operated eye. You need to follow your doctor’s instruction. Any drops you use in your other eye must be continued as normal.
ECP, as well as any laser treatment targeting the ciliary body, causes more inflammation compared to other glaucoma surgery. You will need a few weeks or months of anti-inflammatory eye drop after the procedure.
Most people take 1 – 2 weeks off work after surgery, however the length of time will depend on the nature of your work.
Similar to any procedure targeting at ciliary body (micropulse, HIFU or diode laser), ECP causes inflammation. Combined ECP and cataract surgery will cause more inflammation than routine cataract surgery alone. Your doctor usually gives extra anti-inflammatory medication during the procedure to counter act the inflammatory effect of ECP. Despite this, intense inflammation is always a risk with ECP. This inflammation can occur at the back of your eye (retina), causing a decrease in vision. The loss of vision due to inflammation can be treated and cured with eye drops. However, it may take a few weeks to months for vision to recover.
When there is intense inflammation after surgery, the eye pressure can paradoxically be higher than prior to the surgery. This is usually controlled by an increase in both anti-inflammatory and glaucoma medication. Very rarely, if eye pressure is persistently or extremely high, you will need another glaucoma procedure to control your eye pressure.
Similar to other ciliary body ablation procedures, ECP can lead to extreme low eye pressure and a permanent decrease in vision. This is estimated to happen in less than 5% of patients.
In some cases, ECP may not lower eye pressure or its effect may wear off with time. If ECP fails to lower your eye pressure it will not create any additional harm to your eye. However, you may need to restart your glaucoma medications or have further procedures to control your eye pressure.
There are other forms of laser or ultrasound that target ciliary body to reduce eye pressure (cycloablative procedures): High-intensity Focused Ultrasound (HIFU), micropulse laser and traditional cyclodiode laser.
There are other newer glaucoma procedures that can be performed during cataract surgery such as iStent, Hydrus, XEN Gel Implant or CyPass. These procedures involve inserting a permanent mini stent inside your eye and work at increasing the drainage of fluid.
Other alternatives include simply having cataract surgery alone and continuing to use eye drops to lower eye pressure. A laser procedure called selective laser trabeculoplasty (SLT) also reduces eye pressure by targeting the drainage channels of the eye. SLT is carried out in clinics as an outpatient procedure. The effect of SLT on eye pressure is likely less than ECP and usually has little effect in moderate to advanced glaucoma.
- Francis, B.A., et al., Endoscopic cyclophotocoagulation (ECP) in the management of uncontrolled glaucoma with prior aqueous tube shunt. J Glaucoma, 2011. 20(8): p. 523-7.
- Francis, B.A., et al., Endoscopic cyclophotocoagulation combined with phacoemulsification versus phacoemulsification alone in medically controlled glaucoma. J Cataract Refract Surg, 2014. 40(8): p. 1313-21.
- Francis, B.A., et al., Endoscopic Cycloplasty (ECPL) and Lens Extraction in the Treatment of Severe Plateau Iris Syndrome. J Glaucoma, 2016. 25(3): p. e128-33.
Editors
Founding Editors
MIGS.org was developed by glaucoma surgeons with a broad experience in minimally invasive glaucoma surgery to provide patients with evidence-based and unbiased information.


Glaucoma Specialist
Dr Nathan Kerr