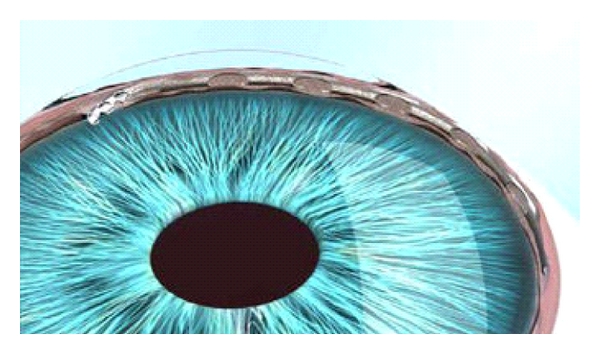
Hydrus Microstent
FAQ
Frequently Asked Questions
The Hydrus Microstent is a tiny scaffold inserted about the size of an eyelash that is inserted into the main drainage channel of the eye to help lower eye pressure and reduce the need for medications. It is so small you will not see or feel it after the procedure. The Hydrus Microstent is made from a super-elastic alloy of nickel and titanium. This material will not cause an allergic reaction and has been used in over a million medical implants. It will not set off airport scanners and is safe if you need to have an MRI scan.
Glaucoma is most commonly associated with a build up of fluid pressure inside the eye. Eye pressure increases because the eye’s fluid drainage channels become blocked. The tiny Hydrus Microstent scaffold is designed to be inserted into the primary fluid canal of the eye and open the channel to allow blocked fluid to flow more freely, thus lowering eye pressure.
The Hydrus is best suited to patients with mild to moderate open-angle glaucoma taking glaucoma drops who are undergoing cataract surgery and wish to reduce their need for glaucoma medications.
The Hydrus is not suitable for advanced glaucoma or where the natural drainage system of the eye is damaged.
The Hydrus helps to reduce the pressure in the eye and may reduce the need or dependence of eye drop medications in patients with mild to moderate glaucoma.
Following combined Hydrus Microshunt insertion and cataract surgery 7 out of 10 patients were medication free at 2 years after surgery compared to only 3 out of 10 patients who had cataract surgery alone.
The Hydrus Microstent will not cure your glaucoma, reverse any damage already caused by glaucoma, or bring back any lost vision.
The Hydrus Microstent is implanted at the end of cataract surgery via the same micro incisions needed for cataract surgery, meaning no additional incisions are necessary. A special injector is used to insert the device into the main fluid drainage canal of the eye, called “Schlemm’s canal”. The operation is usually performed under a local anaesthetic, meaning that you are awake but your eye is numb so you will not feel anything.
The Hydrus Microstent will begin to work straight away to lower your eye pressure and you can stop taking your glaucoma drops in the operated eye. Any drops you use in your other eye must be continued as normal.
Following cataract surgery, you will be given new anti-inflammatory and antibiotic eye drops to use for 4 weeks to prevent inflammation and infection.
Most people take 1 – 2 weeks off work after surgery, however the length of time will depend on the nature of your work.
It is normal for there to be a small amount of bleeding inside the eye during the operation but this resolves within a few days. There is a risk the stent could become blocked or come out of position, however this is rare.
In some cases the Hydrus Microstent may not lower eye pressure or its effect may wear off with time. If the Hydrus Microstent fails to lower your eye pressure it will not create any additional harm to your eye. However, you may need to restart your glaucoma medications or have further procedures to control your eye pressure.
The iStent, Trabectome, and CyPass are alternative minimally invasive procedures that can be performed at the time of cataract surgery to lower eye pressure in patients with primary open angle glaucoma.
Non-surgical alternatives include continuing to use eye drops to lower eye pressure or a laser procedure called selective laser trabeculoplasty.
1. Pfeiffer, N., Garcia-Feijoo, J., Martinez-de-la-Casa, J. M., Larrosa, J. M., Fea, A., Lemij, H., … & Samuelson, T. W. (2015). A randomized trial of a Schlemm’s canal microstent with phacoemulsification for reducing intraocular pressure in open-angle glaucoma. Ophthalmology, 122(7), 1283-1293.
Editors
Founding Editors
MIGS.org was developed by glaucoma surgeons with a broad experience in minimally invasive glaucoma surgery to provide patients with evidence-based and unbiased information.


Glaucoma Specialist
Dr Nathan Kerr